Neuroinflammation is a common thread in neuropathic pain (NP), regardless of the conditions under which neuropathic pain develops. This opens up a whole new avenue for investigations into neuropathic pain pathology. Since the primary cell type responsible for immune-like functions in the CNS is microglia, many researchers have turned their attention toward working to better understand microglial physiology and its potential involvement in neuropathic pain.
[short overview of microglial cells can be found here]
Microglial participation in NP pathophysiology has been investigated using a wide variety of experimental preclinical models. Some of the most common models used are the CCI, SNL and STZ-induced Diabetic neuropathy model. Several lines of evidence compiled using these models have demonstrated the intimate involvement of microglial cells in the establishment of neuropathic pain. More specifically, the process of microglial activation is now thought to be both necessary and sufficient for neuropathic pain initiation. Although there is some variability between results obatined using the different neuropathic pain models, generally microglial cells in the ipsilateral dorsal horn of the spinal cord become activated within approximately 4 hours, increase 2- to 4-fold in number by day 2 and remain active for several months after peripheral nerve injury. These effects can be suppressed by non-specific microglial inhibitors in these preclinical models. In the context of neuropathic pain, local, responding microglial cells are known to be activated by a broad range of stimuli, five predominant activation pathways appear to be most critical and are identified by their major ligand receptor.
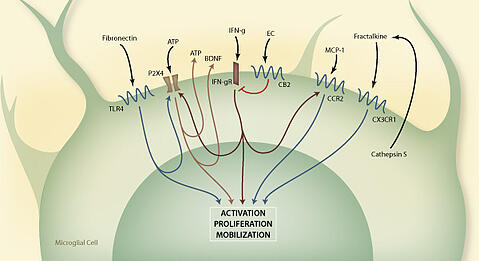
- TLR4 (toll-like receptor family member 4)
- P2X4 (purinociceptor 4)
- INF-g and CB2
- MCP-1
- Fractalkine
These mechanisms have emerged as exciting new focal points for assessing opportunities for the future development of pharmacotherapies, gene therapies or cell-based therapies for neuropathic patients. You can read more about the activation pathways in our new eBook.








